Family-centred practices of healthcare professionals in three emergency departments in KwaZulu-Natal, South Africa
Background. Emergency healthcare professionals can practise family-centred care (FCC) by engaging in active partnerships with families. In a chaotic environment, which challenges communication and supportive behaviours, responding to and acknowledging families’ individuality enhance positive family outcomes.Â
Objective. To describe the adherence of emergency healthcare professionals to family-centred practices in some emergency departments in KwaZulu-Natal, South Africa.Â
Methods. A quantitative survey was conducted among healthcare professionals in three emergency departments. A previously published checklist was used to collect data on adherence to relational and participatory family-centred practices.Â
Results. A total of 77 completed questionnaires were received from the 79 participants surveyed, giving a response rate of 97.5%. Analysis showed that healthcare professionals endeavour to practise FCC, but that their implementation of practice indicators of family-centred care is inconsistent. Results suggested that healthcare professionals used relational practices to a larger extent than participatory practices.Â
Conclusion. In the emergency department, collaboration and partnering with families should be emphasised to ensure that principles of FCC are practised as a standard.Â
Keywords. Family, health care professionals, emergency department, relational practices, participatory practices.
Family-centred care (FCC) is holistic in that it conceptualises illness as a family experience. [1] Effective implementation of FCC involves collaboration between families and healthcare professionals, creating an enabling partnership that respects the sociodemographic diversities of families. [2] Various challenges to the slow evolution of FCC to practice have been cited, with the threat to healthcare professionals’ locus of control superseding all barriers. [3] This may be attributed to difficulties among both organisations and staff to implement a triad of cognitive, behavioural and attitudinal changes. Other challenges include the limited understanding of FCC principles by healthcare professionals and communication difficulties. [4,5]
In South Africa (SA), trauma accounts for the greatest number of unnatural deaths and disabilities in emergency departments (EDs). [6] The initial management of a critical illness occurs in the ED, which results in emergency care and critical care being considered as one in the continuum of acute care. [7] Families and critically ill patients often remain in the ED owing to access block and high bed occupancy in critical care units. [8] Families accompanying their loved ones to the ED are usually unprepared for the turmoil associated with the experience and depend on healthcare professionals to support them through this crisis. [9] To help a patient’s family members to adapt, it is important for healthcare professionals to adhere to relational and participatory family-centred practices. [10,11] Relational practices enable healthcare professionals to build effective and authentic relationships with families; participatory practices are action oriented, aimed at assisting families in capacity building. [11,12] Family-centred practices may appear incompatible with the ED culture, in which objectivity and detachment have priority in clinical decision-making. [13] Healthcare professionals, accustomed to providing life-saving care, need to be quick thinkers who are decisive and in control, [14] and to camouflage the vulnerability that emergency cases may expose them to, they are taught to remain detached lest their emotions interfere with effective decision-making.
Despite the escalation in trauma in SA and the subsequent need to support families in the ED, little research has been conducted on family care in this setting. [15] Relationships with a patient’s family members are shaped by how healthcare professionals perceive the relationship: the more responsive the healthcare professional to the values of FCC, the greater the adherence to family-centred practices. [13,16]
To comment on potential gaps in implementation, this study considered the adherence of emergency healthcare professionals to family-centred practices in three EDs in KwaZulu-Natal, SA.
Methods
Setting and study design
The study was conducted in the EDs of three hospitals in KwaZulu- Natal, SA, using a descriptive survey design. Setting A is a private hospital situated in the eThekwini Metropolitan municipality, Setting B is a state hospital (regional and district) located in the eThekwini health district and Setting C is a state hospital that offers regional and tertiary services to the uMgungundlovu district and the western part of the province. EDs at state hospitals in SA are commonly short staffed, [17] which may impede healthcare professionals’ ability to implement family- centred practices consistently. [18] The settings were specifically chosen with this in mind and to include diversity. All three hospitals have dedicated EDs that provide emergency services to patients with either acute or chronic conditions.
Population, sample and sampling
The population comprised healthcare professionals staffing the three EDs, including: (i) doctors; (ii) nurses registered with the South African Nursing Council as an enrolled nurse with a two-year certificate or as a professional nurse with a diploma or degree in nursing, and (iii) healthcare professsionals with or without a qualification in emergency nursing. On advice from the statistician, all ED staff who met these criteria were invited to participate to accommodate a small population size ( N =82). [19] The sample size ( n =77) derives from sampling of healthcare professionals working in specialised, high-acuity EDs.
The study describes rather than quantifies adherence to family-centred practices in a population of emergency healthcare professionals [20] and forms part of a larger mixed-method interventional study.
Data collection tool
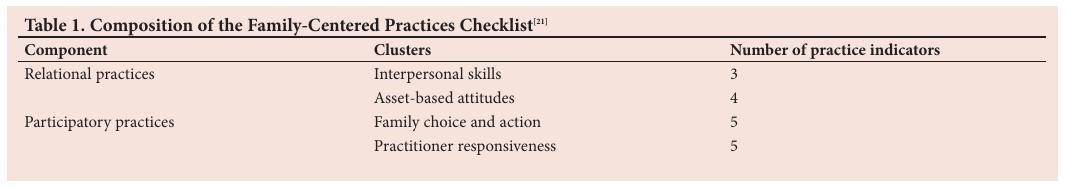
With permission from its developers, the Family-Centered Practices Checklist [21] was administered to healthcare professionals to rate their adherence to 17 practice indicators (PIs). The questionnaire was designed with input from families and healthcare professionals and it enables reflection on practices that occur during interactions between the healthcare professional and the family. The checklist includes a relational component and a participatory component, each of which is divided into two clusters (Table 1). The relational component covers practices that promote effective interaction and the participatory component focuses on family interaction. [21]
PIs were rated according to the following scale:
• 1 – yes, PI was consistently used
• 2 – PI was partially/sometimes adhered to
• 3 – PI not used/opportunity missed
• 4 – not applicable/no opportunity to observe.
The percentage of ‘yes’ responses in the checklist provides a measure of quality regarding family-centred practice, with a lower score indicating greater adherence to family-centred practice. [21] A point of concern for the researcher was that the instrument had no cut-off scores. With the assistance of the statistician, the following denotations were used: a score of 17 indicated total adherence to all PIs, an average of 34 indicated that work still needed to be done to ensure adherence, and a score of 68 indicated no adherence. These interpretations were based on the premise that relational and participatory practices should always be present in interactions between a healthcare professional and a patient’s family. [22] Simple descriptive information was collected with regard to a healthcare professional’s age, gender, qualification and number of years working in the ED.
Validity and reliability
Content validity was achieved through a pilot study with five participants, during which the content was examined for clarity, length and specificity in the SA context. Excellent internal consistency was confirmed (Cronbach’s α = 0.94). Face validity was established through peer review by an emergency nurse specialist and a family nurse specialist.
Data collection process
The researcher contacted the medical and nursing directors of the hospitals and was referred to a liaison within each ED, through whom the researcher met the healthcare professionals. The purpose of the study was explained and healthcare professionals were invited to participate. Written consent was obtained prior to completion of the questionnaire. Data were collected from March to April 2017.
Statistical analysis
Mean scores were calculated for each PI, as well as an overall mean score. Statistical analyses included analysis of variance and an independent sample t -test to assess the influences of demographic variables (gender, age, experience and qualifications of participants) on the overall scores in the four clusters. The Kolmogorov-Smirnov test showed that the scores were normally distributed, which justified the use of the parametric t -test. Significance was set at p< 0.05. Data were computed based on the total number of non-missing cases.
Ethical considerations
Ethical approval for the study was obtained from the university’s Ethics Committee (ref. no. HSS/1731/015D) and the private hospital (ref. no. 20160206). Permission for conducting the study in the state hospitals was obtained from the KwaZulu-Natal Department of Health (ref. no. HR KM44/16 KZ_2016 RP 22_946). Participation in the study was voluntary. An information sheet detailing the right to withdraw from the research and the risk-benefit ratio of the study was attached to the consent form. Confidentiality was assured through coding questionnaires and electronic data were password protected.
Results
A response rate of 97.5% was achieved ( N =77/79).
Demographic characteristics
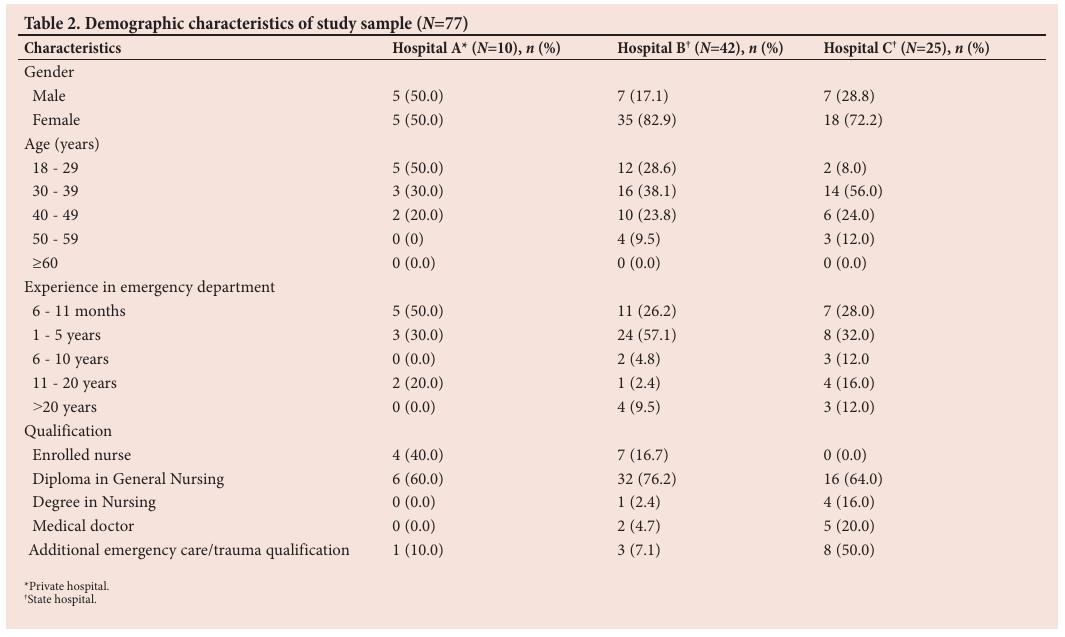
Of the participants, 13.0% ( n =10) were from hospital A, and 54.5% ( n =42) and 32.5% ( n =25) were from hospital B and hospital C, respectively (Table 2). The majority of the participants were female ( n =58; 75.3%). The participants were predominantly between 30 and 39 years of age ( n =33; 42.7%) and had between 1 and 5 years of experience in an ED ( n =35; 45.5%). Nurses comprised 90.9% ( n =70) of the sample. Only 12 participants (15.6%) had an additional qualification in emergency care (Table 2).
Family-centred practices
The average overall score for the checklist was 25.6. The mean score per PI was 1.5. Scores for individual PIs are shown in Tables 3 and 4.
Relational practices component
Interpersonal skills cluster
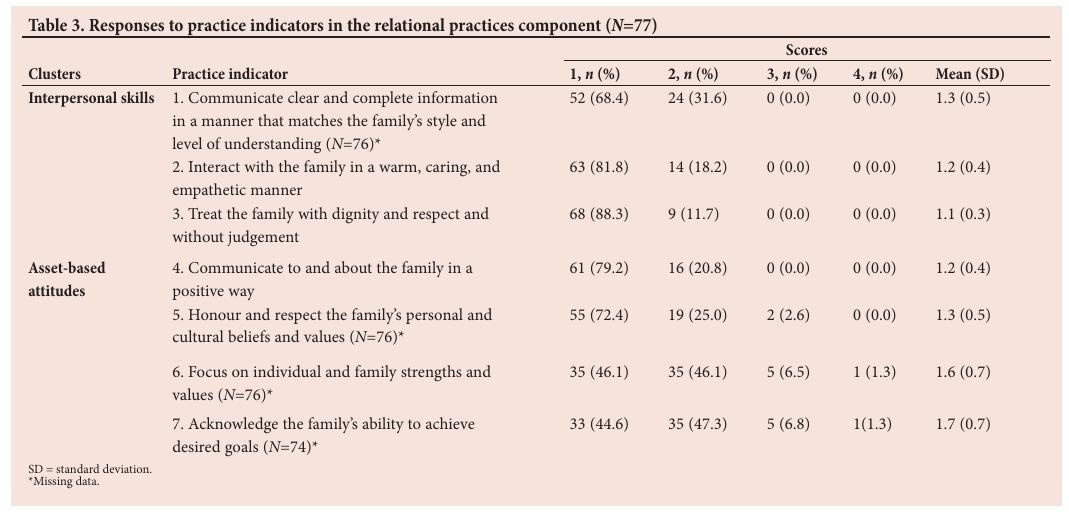
The average score for the cluster was 3.6. The majority of ‘yes’ responses were with regard to treating families non-judgementally and with dignity and respect ( n =68; 88.3%), resulting in a mean score of 1.3.
Asset-based attitudes cluster
The average (mean) score in this cluster was 5.8 (1.2). Communicating positively with families was consistently used by the majority of respondents ( n =61; 79.2%).
Participatory practices component
Family choice and action cluster
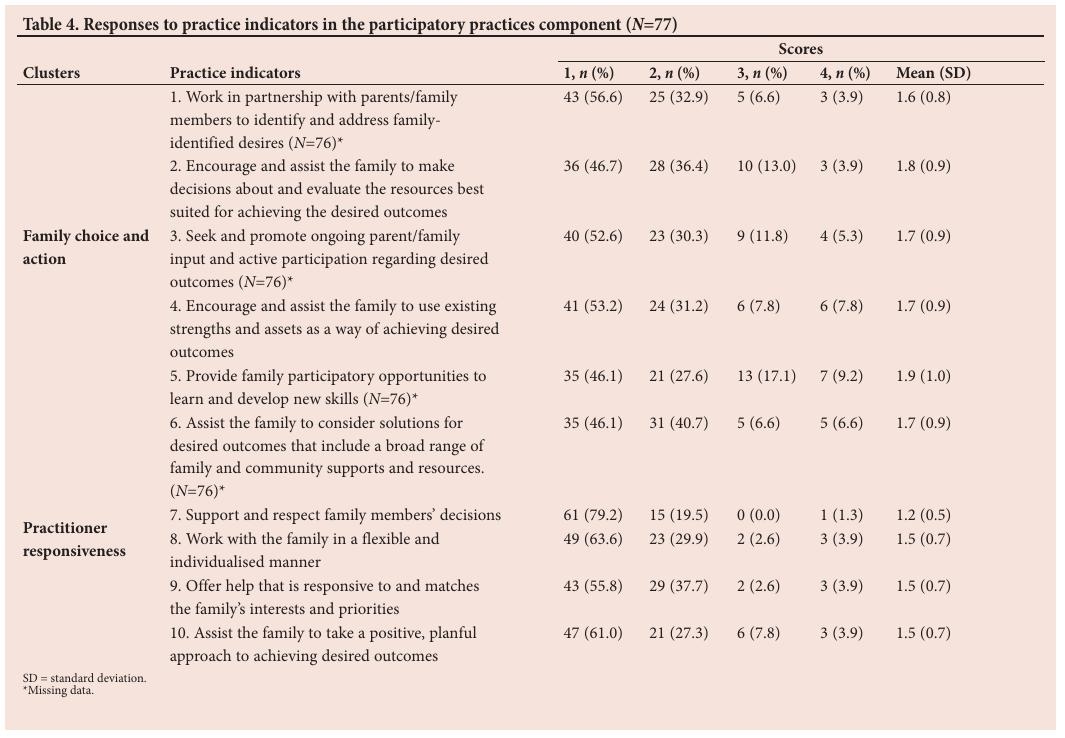
The average score across this cluster was 8.8. Working with families to identify and address their desires was cited as being adhered to most often ( n =43; 56.6%) and was associated with a mean score of 1.6.
Practitioner responsiveness cluster
The average score for the cluster was 7.4. Supporting and respecting families’ decisions was adhered to most often ( n =61; 79.2%) and was associated with a mean score of 1.2.
Demographic influences on the overall scores
within clusters
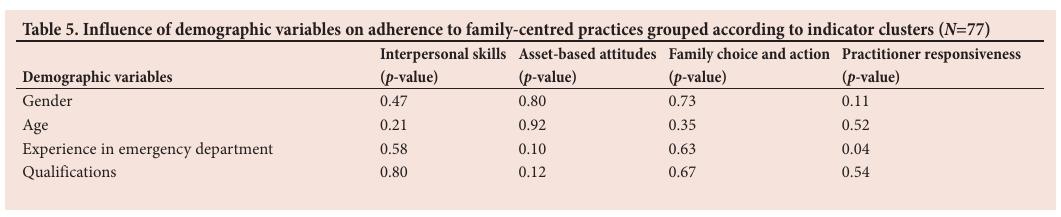
The results revealed a significant difference between years of experience in the ED and the cluster of practitioner responsiveness ( p= 0.04) (Table 5). No statistical variations in the overall cluster scores were evident in the remaining possible associations.
Discussion
Demographic characteristics of participants
Similar to studies from some other developing countries, [10,23] the majority of participants were nurses. This might contribute to FCC in the current setting, as Duran et al . [24] concluded that nurses tend to have a more positive attitude towards family-centred practice than physicians. Family-centred practice
The mean overall score achieved with the checklist indicates that participants did not consistently adhere to the 17 family-centred PIs.
The finding could be attributed to staffing constraints, which remain a challenge in EDs in the SA setting and may have hindered collaboration with families. [9] Such a situation would be of concern, as relational and participatory practices are associated with greater family empowerment. Practitioners’ adherence to relational and participatory practices is essential in building effective partnerships through increased family involvement [25] and positive interactions of this kind lead to effective implementation of family interventions. Although a mean score of 1.5 per PI in the study could be regarded as satisfactory, it indicates that family-centred practices are not consistently adhered to and do not feature in every family interaction. This is similar to a finding by Shields et al. [26] in an Australian study.
Relational practices
Interpersonal skills cluster
The majority of the participants treated families in a dignified and respectful manner. Thébaud et al. [27] note that, as core values in FCC, respect and dignity help to promote partnerships and engagement with families. A similar observation was noted in a Finnish study, [28] where nurses who had to provide emotional support to families of patients with traumatic brain injury reported that they were respectful to families and provided guidance based on their individual circumstances.
Results from the current study show that only 68% of the participants communicated clearly and so provided complete information at a level that families could understand. This is similar to findings in a Brazilian study, in which Zani et al . [29] found that communication between staff and families was not consistent. Communicating accurate information is essential in family–staff interactions as it enables families to exercise autonomy in decision-making. Unclear communication contributes to anxiety and dissatisfaction in patients’ families when they are already stressed. [9]
Asset-based attitudes
Most participants agreed that they communicated to and about the family in a positive way. This is in line with findings by Lukmanulhakim et al ., [30] who reported that nurses in an emergency room in Indonesia displayed active listening skills and were calm and friendly towards families. The authors concluded that the more effective the communication, the less the anxiety of patients’ families. Planned meetings with family members also create opportunities for honest, empathetic communication. [27]
Less than half of the participants in the current study indicated that they always acknowledged the family’s ability to achieve desired goals. The finding is noteworthy, as encouraging an asset-based attitude increases the likelihood that a patient’s family will make progress, gain competence and function more effectively. [31]
Participatory practices
Family choice and action
Responses in this cluster of PIs indicate that the respondents did not always use practices that encourage family participation and decision- making in the illness experience. In a study in Turkey, Shields et al. [5] found that the family of patients in the ED wanted to partner with healthcare professionals, which suggests that participatory practices should be considered when planning FCC. Just over half of the respondents in the current study indicated that they partnered with family members to identify and subsequently address their desires. Shields [32] notes that there is a difference between what families actually need and what healthcare professionals assume they need, and that the mismatch creates discord between family and staff.
Notably, less than half of participants reported that they always provided families with opportunities to participate and develop skills. Although genuine partnerships between families and practitioners are crucial in effective implementation of FCC, [33] care workers tend to be more proficient in relational than participatory practices. Healthcare and allied workers need to be trained to tailor FCC practices to the needs and desires of families and be able to identify the preferences of each family, as this increases trust and indicates respect for the individuality of the family. [4]
Practitioner responsiveness
Most participants stated that they always supported and respected families’ decisions, similar to findings in a study by Gill et al . [34] According to Coco et al. , [28] families often want to make decisions on how they grieve and cope, and this must be acknowledged by practitioners. In a Brazilian study, Baretto et al . [23] reported that systematic work needs to be undertaken so that the family is valued and can collaborate in the emergency process.
Less than half of the participants in the current study reported that they provided resources to help families make decisions. Shields [32] notes that empowering families involves not only meeting their needs but also mobilising resources and support to help them gain control of their lives. In a study by Almaze and De Beer, [35] the majority of emergency nurses agreed that they provided timely, factual information to families, which aided decision-making, and participants in a study by Brysiewicz and Bhengu [4] suggested that social workers and chaplains were needed to provide families with additional support. Interdisciplinary support is especially applicable in the ED, where staff morale can be low and resource constraints may not permit staff to provide adequate support. Demographic influences on practising family-
Demographic influences on practicing family-centred care
Respondents with more extensive ED experience scored worse with regard to practitioner responsiveness. This is contrary to findings reported in other studies. [3,27,36] No statistically significant relationships were found between qualifications, gender or participants’ age and the overall scores in the four indicator clusters. This is contrary to findings from a study in Turkey, where Shields et al. [5] found that practitioners who held a specialist qualification had a better score on working with patients and their families. Similarly, an Australian study revealed that perceptions among ED staff regarding collaborating with families were influenced by education levels, gender and prior experience ( p= 0.05), marital status ( p =0.04) and having children ( p =0.02). [26] In their Irish study, Coyne et al. [3] concluded that nurses with a degree qualification scored better with regard to their perception of FCC than nurses with a certificate qualification. The contrasting findings of the current study are perplexing, and further qualitative inquiry is recommended. However, it has been suggested that specialist education should not include only what FCC entails, but also how to make it work. [26,31,33] Skills training on collaboration with families is also advocated.
Study limitations
Owing to the small sample size, our findings cannot be generalised. Missing data, which may be a result of staff having had to complete the questionnaire while on duty, also impacted on the interpretation of trends.
Conclusion
Results show that healthcare professionals working in the surveyed EDs endeavour to practise FCC, but that their implementation is inconsistent. It is recommend that the Family-Centered Practices Checklist [21] be used regularly as part of practitioners’ reflections on their interactions with families. It can also form part of the assessment of staff’s adherence to family-centred practices and provide focused feedback on areas where guidance and education are needed to strengthen practice.
Acknowledgements. We acknowledge the contribution made by Prof. C Erlingsson.
Author contributions. WE and PB both contributed to the design of the study, data analysis and manuscript preparation. WE completed the data collection and provided statistical support.
Funding. This work was supported by the National Research Foundation/Research and Innovation Support and Advancement (grant number: KFNU2016/02/A13). The publication contents are solely the responsibility of the authors and do not represent official views of any organisation.
Conflicts of interest. None.
1. Eggenberger SK, Sanders M. A family nursing education intervention supports nurses and families in an adult intensive care unit. Australian Critical Care 2016;29:217-223. https://doi.org/10.1016/j.aucc.2016.09.002
2. Shields L, Mamun AA, Pereira S, O’Nions P, Chaney G. Measuring family centred care: Working with children and their parents in a tertiary hospital. Int J Person Cent Med 2011;1(1):155-160. https://doi.org/10.5750/ijpcm.v1i1.41
3. Coyne I, Murphy M, Costello T, O’Neill C, Donnellan C. A survey of nurses’ practices and perceptions of family-centered care in Ireland. J Fam Nurs 2013;19(4):469-488. https://doi.org/10.1177/1074840713508224
4. Brysiewicz P, Bhengu BR. The experiences of nurses in providing psychosocial support to families of critically ill. S Afr J Crit Care 2010;26(2):42-51.
5. Shields L, Çavuşoğlu H, Pars H, Mamun AA. Measuring family-centred care: Working with children and their parents in a Turkish hospital. Eur J Person Cent Healthcare 2015;3(3):327-333. https://doi.org/10.5750/ejpch.v3i3.985
6. Hardcastle TC, Steyn E, Boffard K, et al. Guideline for the assessment of trauma centres for South Africa. S Afr Med J 2011;101(3):189-194. https://doi.org/10.7196/samj.4682
7. Wessman B, Fuller B. Emergency medicine: An integral component of the continuum of critical care that is devalued by fellowship programs. J Emerg Med 2015;49(3):342-344. https://doi.org/10.1016/j.jemermed.2015.03.026
8. Yarmohammadian MH, Rezaei F, Haghshenas A, Tavakoli N. Overcrowding in emergency departments: A review of strategies to decrease future challenges. J Res Med Sci 2017;22(1):23-27. https://doi.org/10.4103/1735-1995.200277
9. Botes M, Langley G. The needs of families accompanying injured patients into the emergency department in a tertiary hospital in Gauteng. Curationis 2016;39(1):1567. https://doi.org/10.4102/curationis.v39i1.1567
10. Chaudhuri S, Malla G, Uprety S, et al. Family presence in emergency: Attitude and belief among health professionals in a tertiary care hospital of Nepal. Health Renaissance 2015;13(3):152-160. https://doi.org/10.3126/hren.v13i3.17963
11. Dunst CJ, Trivette CM, Hamby DW. Meta-analysis of family-centered helpgiving practices research. Ment Retard Dev Disabil Res Rev 2007;13:370-378. https://doi.org/10.1002/mrdd.20176
12. Espe-Sherwindt M. Family-centred practice: Collaboration, competency and evidence. Support for Learning 2008;23(3):136-143. https://doi.org/10.1111/j.1467-9604.2008.00384.x
13. Mentis HM, Reddy M, Rosson MB. Invisible emotion: Information and interaction in the emergency room. Conference on Computer Supported Cooperative Work; 2010 Feb 6-10; Savannah: United States of America.
14. Clarke D, Usick R, Sanderson A, Giles-Smith L, Baker J. Emergency department staff attitudes towards mental health consumers: A literature review and thematic content analysis. Int J Ment Health Nursing 2014;23(3):273-284. https://doi.org/10.1111/inm.12040
15. Wetzig K, Mitchell M. The needs of families of ICU trauma patients. An integrative review. Intensive Crit Care Nurs 2017;41:63-70. https://doi.org/10.1016/j.iccn.2017.02.006
16. Bell JM. Relationships: The heart of the matter in family nursing. J Fam Nurs 2011;17(1):3-10. https://doi.org/10.1177/1074840711398464
17. Van Hoving DJ, Barnetson BK, Wallis LA. Emergency care research priorities in South Africa. S Afr Med J 2015;105(3):202-208. https://doi.org/10.7196/samj.8967
18. Coyne I, O’Neill C, Murphy M, Costello T, O’Shea R. What does family-centred care mean to nurses and how do they think it could be enhanced in practice. J Adv Nursing 2011;67:2561-2573. https://doi.org/10.1111/j.1365-2648.2011.05768.x
19. Israel GD. Determining sample size [fact sheet]. University of Florida; 1992. PEOD-6. https:// www.tarleton.edu/academicassessment/documents/Samplesize.pdf
20. Anderson AJ, Vingrys AJ. Small samples: Does size matter? Invest Ophthalmol Vis Sci 2001;42(7):1411-1413.
21. Wilson LL, Dunst CJ. Checklist for assessing adherence to family-centered practices. http://fipp. org/static/media/uploads/casetools/casetools_vol1_no1.pdf (accessed 14 May 2014).
22. Bell JM, Wright LM. The illness beliefs model: Advancing practice knowledge about illness beliefs, family healing, and family interventions. J Fam Nurs 2015;21(2):179-185. https://doi.org/10.1177/1074840715586889
23. Baretto MDS, De Arruda GO, Garcia-Vivar C, Marcon SS. Family centered care in emergency departments: Perceptions of Brazilian nurses and doctors. Escola Anna Nery 2017;21(2):e20170042. https://doi.org/10.5935/1414-8145.20170042
24. Duran CR, Oman KS, Abel JJ, Koziel VM, Szymanski D. Attitudes towards and beliefs about family presence: A survey of healthcare providers, patients’ families, and patients. Am J Crit Care 2007;16(3):270-279.
25. Coogle CG, Hanline MF. An exploratory study of family-centred help-giving practices in early intervention: Families of young children with autism spectrum disorder. Child Fam Soc Work 2016;21:249-260. https://doi.org/10.1111/cfs.12148
26. Shields L, Smyth W, Mamun A, Lucas L. Working with families in an emergency department: Perceptions of working with children and their parents. Eur J Person Cent Healthcare 2018;6(2):189-195. https://doi.org/10.5750/ejpch.v6i2.1429
27. Thébaud V, Lecorguillé M, Roué JM, Sizun J. Healthcare professional perceptions of family- centred rounds in French NICUs: A cross-sectional study. BMJ Open 2017;7:e013313. https://doi.org/10.1136/bmjopen-2016-013313
28. Coco K, Tossavainen K, Jääskeläinen JE, Turunen H. The provision of emotional support to families of traumatic brain injury patients: Perspectives of Finnish nurses. J Clin Nurs 2013;22:1467-1476. https://doi.org/10.1111/jocn.12136
29. Zani AV, Marcon SS, Tonete VLP, De Lima Parada CMG. Communicative process in the emergency department between nursing staff and patients: Social representations. Online Braz J Nurs 2014;13(2):1-10. https://doi.org/10.5935/1676-4285.20144036
30. Lukmanulhakim S, Anna A. The relationship between communication of nurses and level of anxiety of patient’s family in emergency room dr. Dradjat Prawiranegara hospital, Serang Banten, Indonesia. Int J Res Med Sci 2016;4:5456-5462. https://doi.org/10.18203/2320-6012.ijrms20164228
31. Coyne I. Families and health-care professionals’ perspectives and expectations of family- centred care: Hidden expectation and unclear roles. Health Expect 2015;18:796-808. https://doi.org/10.1111/hex.12104
32. Shields L. What is “family centred care”? Eur J Person Cent Healthcare 2015;3(2):139-144. https://doi.org/10.5750/ejpch.v3i2.993
33. Phiri LM. Assessment of the needs of critically ill/injured patients’ families in an accident and emergency unit. MCur dissertation. Pretoria: University of Pretoria, 2010:1-175. https://repository. up.ac.za/bitstream/handle/2263/26551/dissertation.pdf?sequence=1&isAllowed=y
34. Gill F, Pascoe E, Monterosso L, et al. Parent and staff perceptions of family-centred care in two Australian children’s hospitals. Eur J Person Cent Healthcare 2012;1(2):317-325. https://doi.org/10.5750/ejpch.v1i2.665
35. Almaze JPB, De Beer J. Patient- and family-centred care practices of emergency nurses in emergency departments in the Durban area, KwaZulu-Natal, South Africa. S Afr J Crit Care 2012;33(2):59-65. https://doi.org/10.7196/317
36. Gundo R, Bodole F, Lengu E, Maluwa A. Comparison of nurses’ and families’ perception of family needs in critical care unit at referral hospitals in Malawi. Open J Nurs 2014;4:312-320. https://doi.org/10.4236/ojn.2014.44036
Article Views
Full text views: 3670




1.jpg)
Comments on this article
*Read our policy for posting comments here